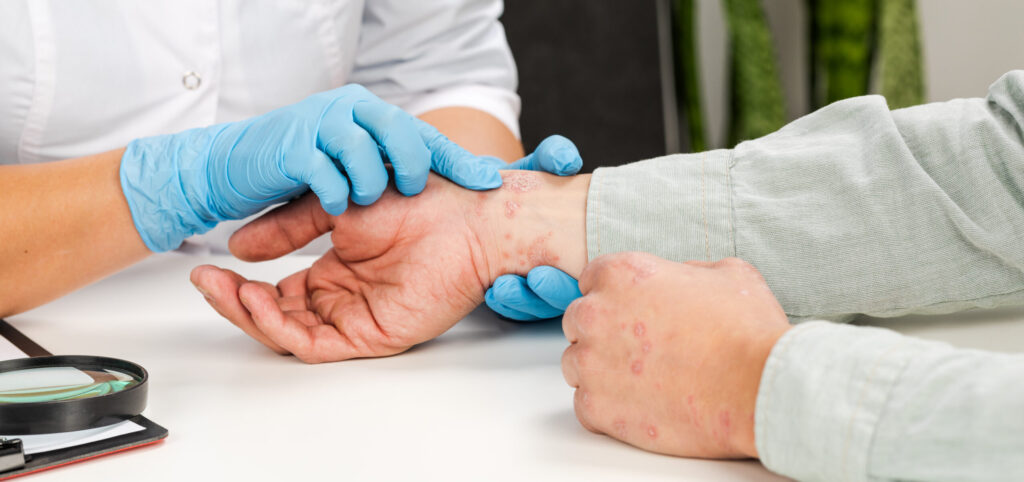
Imagine waking up to dry, itchy patches of skin that seem to come and go with no warning. You try lotions and over-the-counter creams, but nothing seems to keep the redness and discomfort away for good. If this sounds familiar, you’re not alone, and it could be psoriasis.
Psoriasis is a chronic skin condition that affects more than 7.5 million people in the U.S, according to the National Psoriasis Foundation. It’s more than just dry skin; it’s an immune system issue that can affect your skin, joints, and quality of life. The good news? With the right diagnosis and management, you can take control of your symptoms.
What Is Psoriasis?
Psoriasis is a long-lasting (chronic) autoimmune condition that causes skin cells to build up too quickly. This leads to thick, red, scaly patches on the skin that can be itchy, painful, or even crack and bleed. It’s not contagious, and it’s not caused by poor hygiene. Psoriasis is an internal condition that manifests externally.
What Causes Psoriasis?
Psoriasis stems from an overactive immune system that speeds up the life cycle of skin cells. While we don’t fully understand what triggers this immune response, we do know that genetics, environment, and lifestyle all play a role. Common triggers include:
- Stress
- Illness or infection
- Cold or dry weather
- Certain medications
- Skin injuries or sunburns
Types of Psoriasis
There are several types of psoriasis, but the most common is plaque psoriasis. It causes raised, inflamed patches covered with silvery-white scales. Other types include:
- Guttate psoriasis: Small, dot-like spots, often after a strep infection
- Inverse psoriasis: Bright red, shiny lesions in skin folds
- Pustular psoriasis: White, pus-filled blisters surrounded by red skin
- Erythrodermic psoriasis: A severe form with widespread redness and shedding of the skin
Where Does Psoriasis Appear?
Psoriasis can show up almost anywhere, but it most often affects:
- Elbows and knees
- Scalp
- Lower back
- Hands and feet
- Nails (causing pitting or discoloration)
Psoriatic Arthritis: More Than Skin Deep
About 1 in 3 people with psoriasis develop psoriatic arthritis, a condition that causes joint pain, stiffness, and swelling. It most commonly affects the fingers, toes, knees, and lower back. Like psoriasis, psoriatic arthritis is an autoimmune condition, and it can appear before or after skin symptoms begin.
Psoriasis vs. Eczema: What’s the Difference?
While both conditions cause red, itchy skin, they’re not the same. Eczema usually appears earlier in life and is linked more closely to allergies. It tends to cause more oozing and is often triggered by irritants like soaps or fabrics. Psoriasis, on the other hand, is more likely to cause thick, scaly plaques and may be accompanied by joint issues.
Diagnosing Psoriasis
If you suspect you have psoriasis, the best next step is to see a provider. Diagnosis usually involves:
- A physical exam of the skin, scalp, and nails
- A discussion of your medical history and family history
- In some cases, a skin biopsy is needed to rule out other conditions
Managing and Treating Psoriasis
There is no cure for psoriasis, but there are effective ways to manage it. Treatment depends on the type and severity of the condition and may include:
- Topical treatments (like corticosteroids or vitamin D creams)
- Light therapy (UVB treatments)
- Oral or injectable medications that regulate the immune system
- Lifestyle changes (such as managing stress and quitting smoking)
It may take a few weeks to see results, and regular follow-up with a provider is important to find the right treatment plan for you.
Can Psoriasis Be Prevented?
You can’t prevent psoriasis entirely, but you can reduce flare-ups by:
- Avoiding triggers like stress and illness
- Keeping skin moisturized
- Protecting your skin from injury and sunburn
- Following your treatment plan
Living with psoriasis can be frustrating, but with support and the right care, it’s manageable. If you’re experiencing symptoms, don’t wait; talk to a provider to get the answers and relief you need. Early diagnosis and treatment can significantly improve your quality of life.
Our health providers are here to help you stay as healthy as possible. Walk in or reserve a time with Hold My Spot®.
Sources:
National Psoriasis Foundation, Cleveland Clinic, National Psoriasis Foundation, Mayo Clinic, American Academy of Dermatology Association